Educational Information
Your Heart and How it Works
(Source: Heart Rhythm Society https://www.hrsonline.org/Patient-Resources)
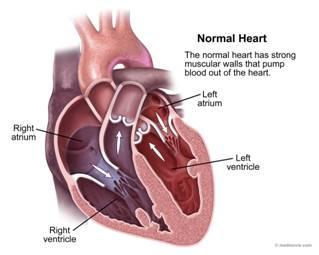
The heart is a fist-sized muscle that pumps blood through the body 24 hours a day, 365 days a year, without rest. The normal heart is made up of four parts: two atria on the top of the heart (right atrium and left atrium), and two ventricles (right ventricle and left ventricle) which are the muscular chambers on the bottom of the heart that provide the major power to pump blood. These four chambers are connected by valves that allow blood to move forward and prevent it from flowing backwards. Coronary arteries, or blood vessels, deliver a constant, nourishing supply of blood to the heart muscle itself.
The heart’s pumping action, or “heartbeat,” is directed by a complicated electrical system. Problems with the regular heartbeat, such as abnormally fast or slow rhythms, can be caused by a heart attack (myocardial infarction) or aging, but may happen for other reasons as well. Heart rhythm problems can cause the feeling that the heart is “racing,” or “skipping” (palpitations), weakness, shortness of breath, passing out (syncope), and sometimes death.
 Blockages in the coronary arteries can also cause major problems in the heart because they slow or stop the flow of blood to the heart muscle. If the heart does not get enough blood, pain (often called angina) or muscle death from a heart attack (myocardial infarction) can result which can damage the heart’s ability to pump and cause abnormal heart rhythms.
Blockages in the coronary arteries can also cause major problems in the heart because they slow or stop the flow of blood to the heart muscle. If the heart does not get enough blood, pain (often called angina) or muscle death from a heart attack (myocardial infarction) can result which can damage the heart’s ability to pump and cause abnormal heart rhythms.
Although people can do a great deal to protect their hearts by exercising regularly, eating a healthy diet, maintaining a healthy weight, not smoking, and controlling their cholesterol and blood pressure, some people are born with a tendency to have heart disease or have other illnesses that may affect the heart.
Arrhythmias and Heart Disease
People with heart disease are at the highest risk for having arrhythmias (abnormal heart rhythms). So, reducing heart disease is important to lowering the risk of arrhythmias. Since the cause of an arrhythmia is not always clear, the best course of action is to prevent and treat heart problems, such as atherosclerosis (“clogged” arteries) and high blood pressure.
- Prevent heart disease by lowering risk factors that can lead to heart disease or cardiac heart rhythm problems, and by monitoring and treating any existing heart problems that you have.
- Make healthy lifestyle choices. Living a “heart healthy” life is the best way to reduce the chances of developing heart disorders. Exercising regularly, maintaining a healthy weight, and eating a healthy, low-fat diet with plenty of vegetables, fruits, and other vitamin-rich foods are the cornerstones of “heart healthy” living.
- Stop smoking and avoid secondhand smoke (smoke from other people). Tobacco contributes to as much as one-third of all heart disease.
- Avoid or limit the intake of caffeine, alcohol, and other recreational drugs.
- Avoid unnecessary stress, such as anger, anxiety, or fear, and find ways to manage or control stressful situations that cannot be avoided.
- Have regular physical exams and tell your doctor right away about any unusual symptoms you may have.
- Talk to a doctor about treating health problems that may contribute to abnormal heart rhythms and heart disease, including atherosclerosis (“clogged” arteries), heart valve damage, high blood pressure, high cholesterol, diabetes, and thyroid disease.
The following conditions can increase the chance of developing arrhythmias, or abnormal heart rhythms:
- Coronary artery disease (blockage in the arteries/pipes of the heart)
- High Blood Pressure
- Diabetes
- Smoking
- High cholesterol
- Obesity/overweight
- A high-fat diet
- Excessive use of alcohol (more than 2 drinks per day)
- Drug abuse
- Stress
- Family history of heart disease
- Advancing age (getting older)
- Sleep apnea
- Certain over-the-counter and prescription medications, dietary supplements, and herbal remedies
 Monitoring and Treating Arrhythmias and Heart Disease
Monitoring and Treating Arrhythmias and Heart Disease
- Effectively treating any existing heart disorder is the best way to prevent it from becoming worse.
- Have regular checkups.
- Understand how some health conditions may increase the risk of abnormal heart rhythms.
- Learn about heart disorders, tests, and treatment options, and talk to your doctor or other health care provider.
- Find out if your heart’s electrical system and its ability to pump blood have been affected by heart muscle damage from a heart attack or another cause.
- Learn the importance of the ejection fraction (EF), which measures the pumping function of the heart. EF is a measure of the proportion, or fraction, of blood the heart pumps out with each beat. (Normal is about 50-70%.) An abnormally low EF is the single most important factor in predicting the risk of sudden cardiac death (dying from an abnormal heart rhythm).
- Follow treatment plans, and take all medications as prescribed.
- Report any new symptoms or changes in existing symptoms to your doctor/health care provider as soon as possible.
Treatment Adherence with Atrial Fibrillation
For patients with Afib, following your treatment plan will reduce your risk of afib-related stroke. Your cardiologist can estimate your risk of a strike using your age, sex, and other medical conditions such as high blood pressure, heart failure, diabetes and vascular diseases. A stroke or mini stroke in the past also increases the risk of having another stroke. Based on your personal risk, your cardiologist may recommend taking a blood-thinning medication to reduce the risk of having a stroke from Afib. Click here for more information on how adhering to your treatment plan is extremely important to reduce your risk of a stroke.
Stroke Prevention is the Cornerstone of Afib treatment
More than three million Americans have Atrial Fibrillation (Afib) which is the most common heart rhythm disorder. People with Afib have a stroke risk five times higher than those who don’t have Afib. Afib causes approximately 120,000 strokes each year. A stroke related to Afib happens when a clot breaks free, lodges in a blood vessel then blocks the flow of blood and oxygen to the brain. One out of every four strokes is due to afib. Click here for more information on Afib and stroke prevention and the role of anticoagulants.
Sleep Apnea and Atrial Fibrillation
About half of patients with Afib also have sleep apnea. Sleep apnea affects about 18 million people in the United States and 100 million worldwide. Sleep apnea is when breathing stops or becomes critically shallow during sleep. Click here for more information on sleep apnea.
Pacemakers
Normally, the heart is signaled to contract, or squeeze, by an electrical impulse that starts in the sinus node at the top of the right atrium. The impulse then travels through the heart’s “wires” to the muscles of the lower chambers of the heart (the right and left ventricles), telling them to contract and cause a heartbeat. This natural system helps the heart pump in an efficient rhythm. A problem with any part of this system, through – either the heart’s natural “pacemaker” or the wires carrying the impulses – can cause a slow heart rate. An artificial pacemaker may be needed to reset the heart to the right pace and make sure blood and oxygen are pumped to the brain and other parts of the body. Click here to read more about what a pacemaker is and how it works.
Want to reduce your risk of heart disease?
The choices we make every day have a lasting effect on our heart and vascular health. Following a healthy eating plan, getting more exercise, avoiding tobacco and managing known risk factors are the recommendations from the American College of Cardiology (ACC) and the American Heart Association (AHA).
Nearly 1 out of 3 deaths for both men and women in the United States is due to heart disease—making it the the leading cause of death in the U.S. The ACC/AHA guidelines say adopting heart healthy habits and doing so over a lifetime is the most important way to prevent cardiovascular disease including whether it’s a build-up of plaque in the arteries, heart attack, stroke, heart failure or issues with how the heart contracts and pumps blood to the rest of the body.
Primary prevention of heart disease starts with an assessment of one’s risk. Patients should frankly and openly talk with their health care team regarding diet, amount of exercise, smoking and any drug use. The guidelines emphasize that a healthy lifestyle is the cornerstone of preventing heart disease. Some of the key lifestyle recommendations are:
- Eating heart healthy – eating more vegetables, fruits, nuts, whole grains and fish and limiting salt, saturated fats, fried foods, processed meats and sweetened beverages. The DASH (Dietary Approaches to Stop Hypertension) is an eating plan to help manage blood pressure and lower the risk of heart disease. See more about the DASH diet at
- https://www.nhlbi.nih.gov/files/docs/public/heart/hbp_low.pdf starting on page 8.
- Exercise regularly – experts recommend getting at least 150 minutes of moderate-intensity exercise such as brisk walking, swimming, dancing or cycling each week. Even 10-minute increments during the day can add up throughout the week. Only half of America adults get the recommended amount of exercise and prolonged periods of sitting can counteract the benefits of exercise.
- Maintain a healthy weight – for people who are overweight or obese, losing just 5% – 10% of their body weight (10-20 pounds for a 200 pound person) can reduce the risk of heart disease, stroke and other health issues.
- Avoiding tobacco by not smoking, vaping or breathing in smoke – 1 in 3 deaths from heart disease is attributed to smoking or exposure to secondhand smoke so every effort should be made to quit. For more information on quitting, go to https://www.lung.org/stop-smoking/i-want-to-quit/.
What is a heart attack?
A heart attack occurs when the blood flow that brings oxygen to the heart muscle is severely reduced or stopped. This happens because coronary arteries that supply the heart with blood can slowly become thicker and harder from a buildup of fat, cholesterol and other substances, called plaque. This slow process is known as atherosclerosis. If the plaque breaks open and a blood clot forms that blocks the blood flow, a heart attack occurs. (Source: American Heart Association.) To see illustrations of how a heart attack occurs, go to: https://watchlearnlive.heart.org/?moduleSelect=hrtatk
Symptoms of a heart attack
(Source: American Heart Association)
Heart attack symptoms can vary from person to person but the most common symptoms are:
- Chest discomfort – most heart attacks involve chest pain (angina) or discomfort in the center of the chest that lasts more than a few minutes or that goes away and comes back. It can feel like uncomfortable pressure, squeezing, fullness or pain.
- Discomfort in other areas of the upper body – symptoms in other areas of the upper body can include pain or discomfort in one or both arms, the back, neck, jaw or stomach.
- Shortness of breath – can occur with or without chest discomfort.
- Other signs may include breaking out in a cold sweat, nausea or lightheadedness. More women than men are likely to experience shortness of breath, nausea/vomiting and back or jaw pain.
Don’t hesitate, call 911! If you feel you may be having a heart attack, don’t wait! Calling 911 is almost always the fastest way to get lifesaving treatment. Emergency medical services (EMS) can begin treatment when they arrive. EMS staff are also trained to revive someone whose heart has stopped.
Stroke Symptoms
(Source: American Heart Association)
To remember how to spot a stroke, think of the acronym F.A.S.T.
- Face drooping – ask the person to smile. Is one side of the face drooping?
- Arm weakness – is one arm weak or numb? Ask the person to raise both arms. Does one arm drift downward?
- Speech difficulty – is speech slurred, are they unable to speak or difficult to understand? Ask the person to repeat a simple phrase such as “the sky is blue” to see if they’re able to repeat it correctly.
- Time to call 911! If the person shows any of these symptoms, even if the symptoms go away, call 911 and get them to a hospital immediately. Time is critical in minimizing the lasting effects of a stroke.
Other stroke symptoms may include sudden confusion, trouble seeing in one or both eyes, sudden trouble walking, dizziness, loss of balance or coordination or a sudden severe headache with no known cause.
For more information on types of stroke and stroke treatment, go to https://www.stroke.org/en/about-stroke/stroke-symptoms/learn-more-stroke-warning-signs-and-symptoms